Understanding Your Sleep Study Report: What the Results Mean

This guide explains what those results typically mean, so they can follow the logic of the report before discussing next steps with a clinician.
What is a sleep study report actually measuring?
A sleep study report explains how they sleep and how their body functions during sleep, with a particular focus on breathing and oxygen levels. Most reports combine data on brain activity, breathing effort, airflow, oxygen saturation, heart rate, and body movements to provide a comprehensive overview.
Depending on the type of test performed, the report may be based on a home sleep apnoea test (HSAT) or an in-lab polysomnography (PSG). In-lab reports are generally more detailed because they measure and classify actual sleep stages in addition to breathing patterns.
Which type of sleep study did they have, and why does it matter?
It matters because HSAT estimates sleep using recording time, while PSG measures sleep directly. That difference can change how indices are calculated and how confident a diagnosis is.
HSAT is commonly used when obstructive sleep apnoea is strongly suspected. PSG is often used when results are unclear, symptoms do not match HSAT findings, or when other conditions like parasomnias, narcolepsy, or periodic limb movement disorder are being considered.
Table of Contents
ToggleWhat do “sleep stages” and “sleep architecture” mean in the report?
They describe how their sleep is divided across the night, usually into N1, N2, N3 (deep sleep), and REM sleep. A typical report shows time and percentage in each stage, plus a chart (hypnogram) of how stages change.
More fragmented sleep often shows as frequent awakenings, lots of light sleep (N1), and reduced deep or REM sleep. One abnormal night is not always meaningful, but patterns can explain symptoms like unrefreshing sleep.
What does “sleep efficiency” tell them?
Sleep efficiency is the percentage of time in bed (or recording time) spent asleep. Lower sleep efficiency usually means more time awake, more awakenings, or difficulty falling asleep.
Many labs flag low sleep efficiency because it can worsen daytime tiredness even when breathing indices are mild. It can also reduce REM sleep, which is important because breathing events sometimes cluster in REM.
What are apnoeas, hypopnoeas, and respiratory events?
They are breathing disturbances during sleep that can reduce airflow, oxygen, or cause arousals. An apnoea is typically a near-complete pause in airflow, while a hypopnoea is a partial reduction.
Reports may also include RERAs (respiratory effort-related arousals), which are subtler breathing events that fragment sleep. The exact definitions can vary slightly by lab rules, so the report’s scoring criteria matter.
What do AHI and RDI mean, and what is “normal”?
AHI (Apnoea–Hypopnoea Index) is the average number of apnoeas and hypopnoeas per hour of sleep (PSG) or per hour of recording (HSAT). RDI (Respiratory Disturbance Index) usually includes additional events like RERAs.
Many reports classify obstructive sleep apnoea severity roughly as: mild (5–14), moderate (15–29), severe (30+). “Normal” is often below 5, but symptoms, oxygen drops, and arousals still matter. Click here to get more about sleep apnea test Adelaide: 5 signs You should book one.
What is the difference between obstructive and central sleep apnoea in the results?
Obstructive events happen when the airway narrows or collapses while breathing effort continues. Central events happen when the brain temporarily reduces the drive to breathe, so effort drops too.
Most reports break events down into obstructive apnoeas, central apnoeas, mixed apnoeas, and hypopnoeas. A clinician looks at the pattern and proportion because treatment differs, especially if central events are prominent.
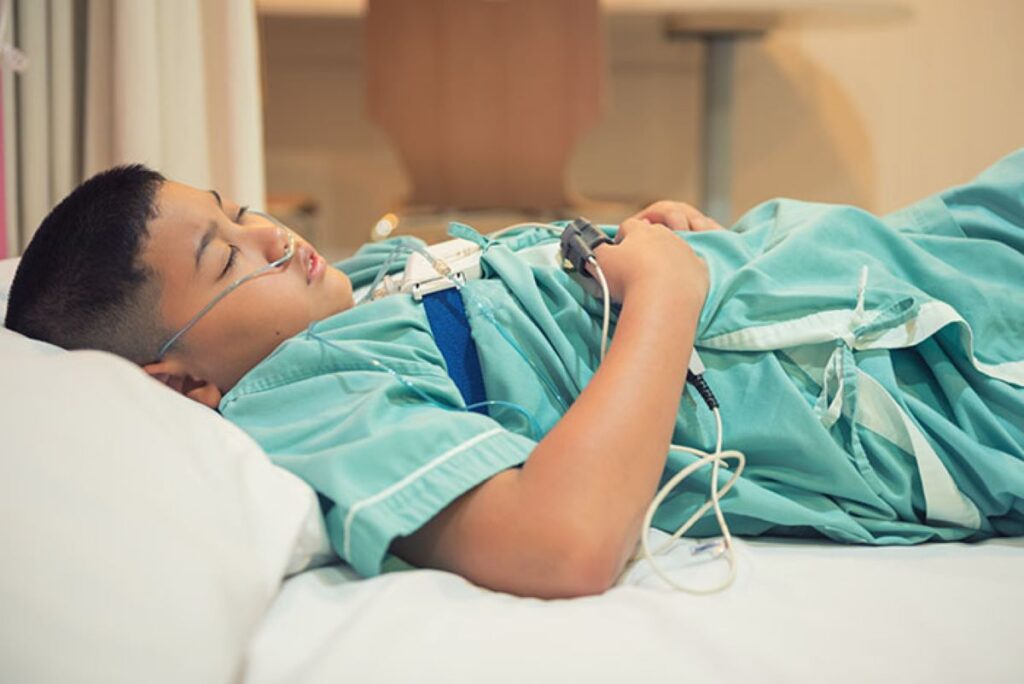
What does the oxygen section (SpO₂) mean for their health?
It shows how well oxygen levels stayed up during sleep and how often they dipped. Key values usually include baseline/mean SpO₂, the lowest SpO₂ (nadir), and time spent below thresholds such as 90%.
Brief dips can still be significant if they happen repeatedly. A low nadir or substantial time below 90% often pushes clinicians to treat more urgently, particularly in people with heart or lung conditions.
What is ODI, and why might it look different from AHI?
ODI (Oxygen Desaturation Index) counts how many oxygen drops occur per hour, often using a 3% or 4% drop rule. It can be lower than AHI if many breathing events cause arousals without major oxygen drops.
It can also be higher than AHI if oxygen drops occur for reasons other than scored apnoeas or hypopnoeas. Comparing AHI and ODI helps clinicians see whether events are mainly desaturation-driven or arousal-driven.
Other Resources : Understanding the sleep cycle
What do arousals and awakenings mean, and why do they matter?
Arousals are brief disruptions in sleep that can prevent deep, restorative sleep, even if they do not fully wake them. Reports may list an arousal index (arousals per hour) and sometimes link arousals to breathing, movement, or spontaneous causes.
High arousal rates often explain fatigue, headaches, poor concentration, and mood changes. Someone can have a borderline AHI but still feel awful if sleep is repeatedly fragmented.
What do heart rate and rhythm findings usually indicate?
Most sleep studies track heart rate and may note irregular rhythms. Many reports simply show average and range, but some include comments on ectopic beats or suspected atrial fibrillation patterns.
An elevated heart rate during clusters of breathing events can support the idea that apnoea is stressing the cardiovascular system. If the report flags rhythm concerns, it usually prompts follow-up rather than providing a definitive cardiac diagnosis.
What do limb movements (PLMS) mean in the report?
PLMS (Periodic Limb Movements in Sleep) are repetitive leg movements that can fragment sleep. Reports may show a PLM index and a PLM arousal index, which is often the more important number.
PLMS can occur on their own or alongside conditions like restless legs syndrome. Treatment decisions typically depend on symptoms, sleep disruption, iron status, and whether breathing events are also present.
What is body position data, and why does it change the interpretation?
Position data shows whether events are worse on the back (supine) versus side or front. Many people have “positional” obstructive sleep apnoea, where AHI is significantly higher when supine.
If the report shows a strong positional pattern, clinicians may discuss side-sleeping strategies, positional devices, or targeted therapy. It also helps explain why symptoms can vary night to night.
What does REM-related sleep apnoea mean?
It means breathing events cluster mainly during REM sleep. This can happen even when the overall AHI looks mild because REM can make the airway more collapsible.
REM-related apnoea may still cause significant oxygen dips and vivid sleep disruption. It is especially relevant if the study captured little REM, because limited REM can underestimate severity.
How do they know if the results match the symptoms?
They compare the numbers with the clinical picture: snoring, witnessed pauses, choking awakenings, daytime sleepiness, morning headaches, and concentration problems. They also consider comorbidities like hypertension, diabetes, reflux, or depression.
A report can look “mild” but still justify treatment if symptoms and oxygen findings are significant. Conversely, some people with higher AHI may report fewer symptoms, and treatment choices may prioritise long-term risk reduction.

What do common recommendations (CPAP, APAP, oral appliance) mean?
They are options to keep the airway open and improve sleep quality. CPAP provides fixed pressure, while APAP adjusts within a range; reports may recommend pressure settings or a trial.
Oral appliances reposition the jaw and can help in mild to moderate obstructive sleep apnoea, especially if they cannot tolerate CPAP. Recommendations often also include weight management (if relevant), avoiding alcohol near bedtime, and treating nasal obstruction.
What should they ask at the follow-up appointment?
They should ask which result drove the diagnosis, whether the test likely underestimated severity, and what success looks like in their case. They can also ask how to measure improvement: symptoms, device data, repeat testing, or blood pressure changes.
Helpful questions include: which events were obstructive versus central, whether oxygen dips were concerning, whether sleep was fragmented by arousals, and whether position or REM made it worse. The goal is a plan that fits both the numbers and how they feel.
FAQs (Frequently Asked Questions)
What does a sleep study report measure and why is it important?
A sleep study report measures how a person sleeps and how their body behaves during sleep, focusing on breathing, oxygen levels, brain activity, heart rate, and movement. This comprehensive data helps clinicians understand sleep quality and diagnose conditions like obstructive sleep apnoea or other sleep disorders.
How do home sleep apnoea tests (HSAT) differ from in-lab polysomnography (PSG) in sleep studies?
HSAT estimates sleep based on recording time and is typically used when obstructive sleep apnoea is strongly suspected. PSG measures actual sleep stages directly in a lab setting, providing more detailed information useful for unclear cases or when diagnosing complex conditions like parasomnias or narcolepsy.
What are sleep stages and how do they affect the interpretation of a sleep study report?
Sleep stages refer to the division of sleep into N1, N2, N3 (deep sleep), and REM phases. Sleep architecture shows the time spent in each stage and patterns throughout the night. Fragmented sleep with frequent awakenings or reduced deep/REM sleep can explain symptoms such as unrefreshing rest.
What is Apnoea–Hypopnoea Index (AHI) and Respiratory Disturbance Index (RDI), and what do their values indicate?
AHI measures the average number of apnoeas and hypopnoeas per hour of sleep or recording; RDI includes additional events like respiratory effort-related arousals (RERAs). Severity is classified as mild (5–14), moderate (15–29), or severe (30+), with values below 5 generally considered normal but symptoms and oxygen drops also influencing diagnosis.
How do obstructive and central sleep apnoea differ in a sleep study report?
Obstructive apnoeas occur when the airway narrows or collapses despite continued breathing effort, while central apnoeas happen when the brain temporarily reduces breathing drive, causing decreased effort. Differentiating these types is crucial as treatment approaches vary significantly depending on the dominant event type.
Why are oxygen saturation levels (SpO₂) critical in interpreting a sleep study report?
SpO₂ levels indicate how well oxygen is maintained during sleep. Key metrics include baseline/mean saturation, lowest saturation (nadir), and time spent below thresholds like 90%. Frequent or prolonged dips can signal serious health risks requiring urgent treatment, especially in individuals with heart or lung conditions.
This guide explains what those results typically mean, so they can follow the logic of the report before discussing next steps with a clinician. What is a sleep study report actually measuring? A sleep study report explains how they sleep and how their body functions during sleep, with a particular focus on breathing and oxygen…
Recent Posts
 Home vs. Portable: Can One Oxygen Concentrator Do Both?Home vs. Portable: Can One Oxygen Concentrator Do Both? For many Australians managing chronic respiratory conditions like COPD or emphysema, the quest for the “perfect” oxygen setup often leads to one critical question: Can one oxygen […]
Home vs. Portable: Can One Oxygen Concentrator Do Both?Home vs. Portable: Can One Oxygen Concentrator Do Both? For many Australians managing chronic respiratory conditions like COPD or emphysema, the quest for the “perfect” oxygen setup often leads to one critical question: Can one oxygen […] Understanding Your Sleep Study Report: What the Results MeanThis guide explains what those results typically mean, so they can follow the logic of the report before discussing next steps with a clinician. What is a sleep study report actually measuring? A sleep study report explains how they sleep and how their […]
Understanding Your Sleep Study Report: What the Results MeanThis guide explains what those results typically mean, so they can follow the logic of the report before discussing next steps with a clinician. What is a sleep study report actually measuring? A sleep study report explains how they sleep and how their […] Sleep Apnea Test Adelaide: 5 Signs You Should Book OneIf they live in Adelaide and recognise the signs below, booking a sleep apnoea test is often the fastest way to get clarity and start feeling better. What exactly is sleep apnoea, and why does testing matter? A sleep apnea test Adelaide service is used […]
Sleep Apnea Test Adelaide: 5 Signs You Should Book OneIf they live in Adelaide and recognise the signs below, booking a sleep apnoea test is often the fastest way to get clarity and start feeling better. What exactly is sleep apnoea, and why does testing matter? A sleep apnea test Adelaide service is used […] Ultimate Guide to Choosing an Oxygen Concentrator in Australia (2026)ntroduction to Modern Oxygen Therapy For many Australians living with chronic respiratory conditions, maintaining an active lifestyle in cities like Sydney requires more than just medical advice—it requires the right technology. An oxygen concentrator is […]
Ultimate Guide to Choosing an Oxygen Concentrator in Australia (2026)ntroduction to Modern Oxygen Therapy For many Australians living with chronic respiratory conditions, maintaining an active lifestyle in cities like Sydney requires more than just medical advice—it requires the right technology. An oxygen concentrator is […] The Best CPAP Mask Options for New Users and What Makes Them ComfortableSleep apnea disrupts breathing during sleep, causing repeated pauses that prevent restful sleep and strain the cardiovascular system. CPAP therapy delivers continuous pressurized air through a mask, keeping airways open throughout the night and enabling […]
The Best CPAP Mask Options for New Users and What Makes Them ComfortableSleep apnea disrupts breathing during sleep, causing repeated pauses that prevent restful sleep and strain the cardiovascular system. CPAP therapy delivers continuous pressurized air through a mask, keeping airways open throughout the night and enabling […] Oxygen Machine for Home Use: A Complete Guide for First-Time BuyersWhat Is an Oxygen Machine and How Does It Work? An oxygen machine for home use, commonly known as an oxygen concentrator, is a medical device that delivers concentrated oxygen to individuals with respiratory conditions. These respiratory therapy devices […]
Oxygen Machine for Home Use: A Complete Guide for First-Time BuyersWhat Is an Oxygen Machine and How Does It Work? An oxygen machine for home use, commonly known as an oxygen concentrator, is a medical device that delivers concentrated oxygen to individuals with respiratory conditions. These respiratory therapy devices […] Medical Oxygen at Home: Essential Information on Oxygen Tanks, Machines, and TherapiesIntroduction For individuals with chronic respiratory conditions, such as COPD, asthma, or emphysema, medical oxygen therapy at home is often a critical part of maintaining health and improving quality of life. Whether you need an oxygen machine for […]
Medical Oxygen at Home: Essential Information on Oxygen Tanks, Machines, and TherapiesIntroduction For individuals with chronic respiratory conditions, such as COPD, asthma, or emphysema, medical oxygen therapy at home is often a critical part of maintaining health and improving quality of life. Whether you need an oxygen machine for […] Understanding Sleep Apnea: Causes, Symptoms, and Effective TreatmentsSleep is one of the most vital pillars of good health, but for millions of people, restful sleep is harder to achieve than it should be. One of the most common reasons for poor sleep quality is sleep apnea, a potentially serious sleep disorder that often […]
Understanding Sleep Apnea: Causes, Symptoms, and Effective TreatmentsSleep is one of the most vital pillars of good health, but for millions of people, restful sleep is harder to achieve than it should be. One of the most common reasons for poor sleep quality is sleep apnea, a potentially serious sleep disorder that often […] Bulk-Bill Sleep Study Brisbane: Affordable Options for LocalsWhat Are Bulk-Bill Sleep Studies and How Do They Work in Brisbane? Bulk-bill sleep study Brisbane services provide you with direct billing to Medicare, eliminating upfront costs for diagnostic testing. When you receive a bulk-bill sleep study, the […]
Bulk-Bill Sleep Study Brisbane: Affordable Options for LocalsWhat Are Bulk-Bill Sleep Studies and How Do They Work in Brisbane? Bulk-bill sleep study Brisbane services provide you with direct billing to Medicare, eliminating upfront costs for diagnostic testing. When you receive a bulk-bill sleep study, the […] Sleep Apnea Test Adelaide: Early Diagnosis for Better HealthWhat Is Sleep Apnea and Why Is Early Diagnosis Important? Sleep apnea is a serious sleep disorder where your breathing repeatedly stops and starts during sleep. This condition affects millions of people worldwide, yet many remain undiagnosed, missing […]
Sleep Apnea Test Adelaide: Early Diagnosis for Better HealthWhat Is Sleep Apnea and Why Is Early Diagnosis Important? Sleep apnea is a serious sleep disorder where your breathing repeatedly stops and starts during sleep. This condition affects millions of people worldwide, yet many remain undiagnosed, missing […]
Categories
- CPAP Machine
- CPAP Mask Online
- CPAP Masks
- Cpap Masks Australia
- Laser Eye Surgery
- Lasik Surgery
- Medical Oxygen
- Oxygen Concentrator
- Portable Oxygen Concentrator Australia
- Portable Oxygen Concentrator Machine
- ResMed AirMini
- Sleep Apnea
- Sleep Apnea Test Adelaide
- Sleep Apnea Test Brisbane
- Sleep Study
- Sleep Type Test
- Sydney Eye Clinic
